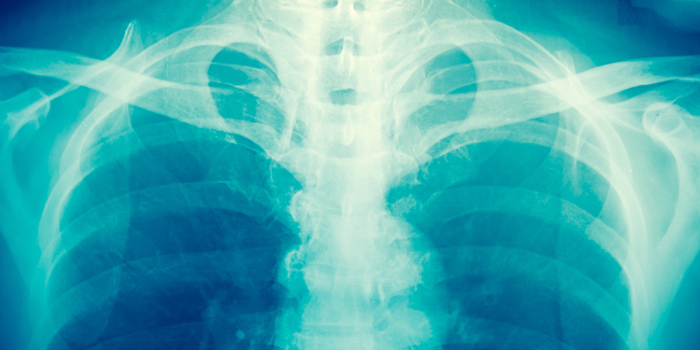
X-ray
Also known as radiography, X-rays are the oldest medical imaging modality. They have been in use since 1895 when they were discovered by a German physicist named Wilhelm Conrad Roentgen. A beam of x rays passing through a specific part of a patient’s body is used to produce the X-ray image. As the x rays pass through the body they will be blocked to different degrees by the different organs of the body. The x-ray beams that do get through are captured on a detector that is placed on the other side of the patient. A radiographic image is then produced from the beams that are captured on the detector.
Baylor Radiologists use X-ray to report both normal and abnormal conditions in the body. The most commonly obtained plain films are generally of the chest, abdomen and bones. Plain films may aid in the diagnosis of chest, abdominal or joint pain, difficulty breathing, fever, vomiting and traumatic injury diagnosing conditions such as pneumonia, congestive heart failure, fractures and arthritis. During the examination the patient will be positioned appropriately between the x ray tube and the electronic detector system by the technologist. Care will be taken to ensure that the x ray beam is directed only to the body part being imaged. For certain examinations, multiple images may be obtained.
The images obtained are then processed and sent to the radiologist for review, interpretation and reporting. The exam generally takes only a few minutes.
Common uses for general X-ray technology include the diagnosis of
- Pneumonia
- Congestive heart failure
- Bone fractures
- Arthritis
Click below for additional information:
Fluroscopy
Fluroscopy utilizes x-ray beams to view “realtime” images on a video monitor of organs that may or not have been enhanced by contrast administration. Important images are then captured during the examination. Fluoroscopy has many applications in radiology include evaluation of the gastrointestinal tract and urinary tract and for the performance of procedures such as lumbar punctures.
Common uses for fluoroscopy include:
- Upper gastrointestinal series to evaluate patients with suspected gastro-esophageal reflux and other problems such as swallowing difficulty.
- Screen patients for ulcers, benign tumors/polyps, cancer, or certain intestinal illnesses.
Click below for additional information:
Joints (Arthrography)
Lower GI/Barium Enema
Myelography
Upper GI
CT
X-rays are used in conjunction with advanced detectors and computers to create images for CT scans. Frequently, CT is performed in conjunction with the intravenous administration of iodinated contrast as well as the ingestion of oral contrast. The intravenous contrast is a clear fluid that allows better visualization of the body’s internal organs. The oral contrast outlines the gastrointestinal system. Together, the contrast help the Singleton radiologist interpret an examination, The patient slides through a doughnut like machine while lying on a table. The process is rarely uncomfortable and imaging acquisition itself usually takes less than 5-10 minutes.
If a patient cannot receive iodinated contrast because of allergy, an MRI is usually ordered.
Common uses of a CT scan include the following procedures:
- CT of the chest is used to detect lung disease, pneumonia, or lung masses.
- CT colonography can be used to screen patients for colon cancer especially in patients that can not tolerate traditional colonoscopy exams or have incomplete colonoscopies.
- CT body scans are commonly used to detect tumors and monitor a patient’s response to various treatments.
- CT scanning can also be used to guide procedures such as the biopsy of lung, liver, lymph nodes, kidneys, pancreas, etc as well as to aspirate or drain infected or non-infected fluid collections in the abdomen and pelvis.
Click below for additional information:
Abdomen and Pelvis
Body
Chest
Virtual Colonoscopy
Head
Percutaneous Abscess Drainage
Needle Biopsy of Lung Nodules
Sinuses
Spine
MRI
MRI scanning uses radio waves, a large electromagnet and computers to generate images. Certain adjustments in the equipment are made to image the same regions in different ways to look for different types of abnormality. An MRI machine is composed of a large box with a central tube into which the patient is placed. For some individuals, the tube may feel confining and some patients therefore require sedatives in order to allow them to remain still. Studies often take a total of 30 to 60 minutes complete. Gadolinium intravenous contrast is often given which allows our radiologist to visualize certain organs and disease conditions better.
Clinical Instructions
A pregnancy test may be necessary prior to your MRI exam. The risks to a fetus are unknown. Therefore, pregnant women should not have an MRI exam unless the potential benefit from the MRI is determined to outweigh the potential risks. If you have minor claustrophobia (fear of enclosed spaces) or anxiety, you may want to request a prescription for a mild sedative from your physician. If you have an allergy of any kind such as hay fever, hives, allergic asthma, or allergy to food or drugs, please indicate that on your history form as rarely, some individuals can have an allergy to gadolinium. However, gadolinium does not contain iodine and is less likely to cause an allergic reaction as compared to the CT contrast that contains iodine. The technologist and radiologist should also know if you have any significant health problems. Some conditions, such as kidney disease and sickle cell anemia, may prevent you from having an MRI with contrast material.
Metal and electronic objects can interfere with the MRI’s magnetic field and are not allowed in the exam room. These items include:
- Jewelry, credit cards, watches, hearing aids, all of which can be damaged.
- Pins, hairpins, metal zippers and similar metallic items, which can distort MRI images.
- Removable dental work.
- Pens, pocketknives and eyeglasses.
In most cases, an MRI exam is safe for patients with metal implants, except for a few types.
Tell the technologist if you have medical or electronic devices in your body, such as artificial heart valves, implanted drug infusion ports, implanted electronic devices, artificial limbs or metallic joint prostheses, implanted nerve stimulators, metal pins, screws, plates or surgical staples.
Metal objects used in orthopedic surgery usually pose no risk during MRI. However, a recently placed artificial joint may require the use of another imaging procedure such as CT. If there is any question, an x-ray may be taken to detect the presence of any metal objects.
Common uses of MR imaging include the following:
- Body MR imaging is used to detect and further characterize lesions in kidney, liver, pancreas, spleen and adrenal glands. MRI is also often used to characterized ovarian masses/cysts as well as uterine fibroids.
- Musculoskeletal MR imaging is used to evaluate, diagnose, and monitor treatment response of the body joints, spine, and soft tissues of the extremities.
- Breast MR imaging supplements mammography and ultrasound imaging for the diagnosis of breast abnormalities.
Click below for additional information:
Body
Cardiac
Chest
Head/Brain
Musculoskeletal
Spine
MRCP (Magnetic Resonance Cholangiopancreatography)
MR Angiography
Breast
Uterine Fibroid Embolization (UFE)
Ultrasound
Ultrasound uses a handheld transducer that emits high frequency sound waves and receives the echoes created by the body to generate an image. The procedure is quick and painless. It does not use radiation making it ideal in the pediatric population and in pregnant women. A lubricant gel is placed on the skin to allow the waves to pass through the skin and into body parts and organs that are being examined.
Common uses for Ultrasound imaging technology includes:
- Symptom evaluations
- Examination of the body’s internal organs
- Female reproductive examinations
- Guide biopsies
MRA/CTA
Computed tomographic angiography (CTA) and magnetic resonance angiopgrahy (MRA) are non-invasive ways for evaluating the blood vessels in the body with a CT or MRI scanner. Contrast material is injected at a relatively rapid rate through an IV line. With the latest CT and MRI scanners, fine detailed images of the vessels are obtained. CTA and MRA can be used to diagnose coronary artery blockage/narrowing, aortic dissections or aneurysms among many of the other disease processes affecting the vasculature.
Click below for additional information:
Coronary Computed Tomography Angiography (CTA)
CT Angiography (CTA)
MR Angiography (MRA)
Interventional
Interventional radiology is a general term that refers to several different procedures that utilize a while host of different modalities within the field of radiology including fluoroscopy, ultrasound, CT and MRI to diagnose and treat many disease conditions. Most procedures utilize a tiny opening within the body often created by small needle. Many of the diagnostic and therapeutic procedures within interventional radiology are an alternative to surgical procedures.
Click below for additional information:
Catheter Angiography
Angioplasty and Vascular Stenting
Catheter Directed Thrombolysis
Dialysis and Fistula Declotting and Interventions
Inferior Vena Filter Placement and Removal
Intracranial Vascular Treatments
Transjugular Intrahepatic Portosystemic Shunt
Biliary Interventions
Bone Densitometry
Bone densitometry (also known as Dual energy x-ray absorptiometry (DEXA)) is today’s established standard for measuring bone mineral density (BMD). IT is a painless and quick procedure for measuring bone loss. Measurement of the lower spine and hips are most often done. DEXA bone densitometry is used to diagnose osteoporosis and assess a patient’s risks for developing fractures. Unlike plain film x-rays, it will not tell whether you will or will not have a fracture. Rather, it gives a relative risk of suffering a fracture. A low reading should not cause you to be anxious but may help you set healthy goals. If your bone density is found to be low, you and your physician can work together on a treatment plan to help prevent fractures before they occur. DEXA is also effective in tracking the effects of treatment for osteoporosis or for other conditions that cause bone loss.
Clinical Instructions
On the day of the exam eat normally, but don’t take calcium supplements for at least 24 hours beforehand. Wear loose, comfortable clothing, avoiding garments that have zippers, belts or buttons made of metal. Inform your physician if you recently had a barium examination or have been injected with a contrast material for a computed tomography (CT) scan or radioisotope scan; you may have to wait 10 to 14 days before undergoing a DEXA test. Women should always inform their physician or x-ray technologist if there is a possibility they are pregnant.
For additional information, click the links below: