Baylor Radiologists uses several different imaging modalities including mammography, ultrasound and MRI to evaluate the breasts. Generally, mammography is used as the initial screening test.
Mammography
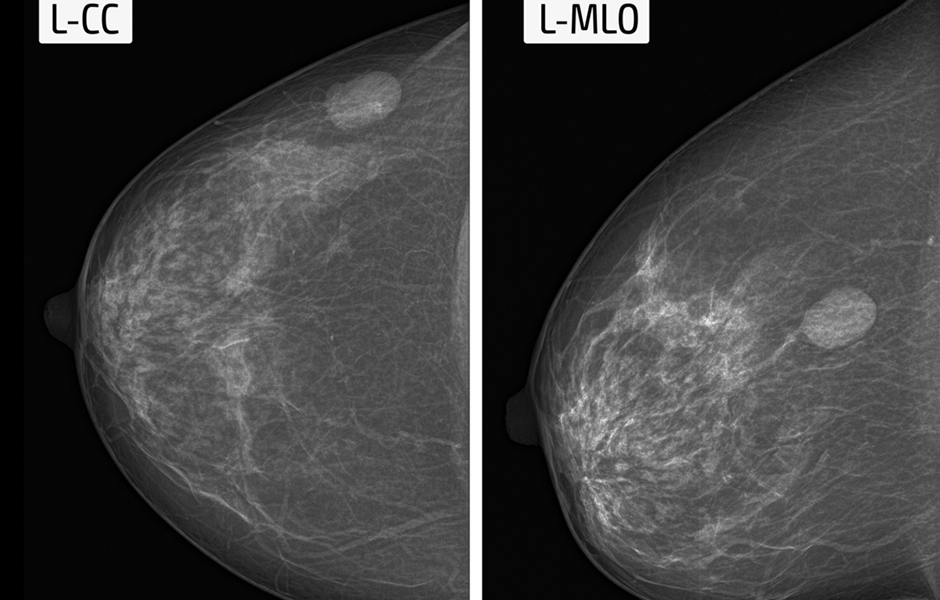
Screening mammography usually consists of 2 views of each breast and can assist your physician in the detection of breast cancer. Yearly mammograms can lead to early detection of breast cancers. Early detection of breast cancer makes it more curable and usually make breast-conservation therapies more likely. In addition, yearly mammography is the only screening tool shown to decrease breast cancer mortality rates. If a finding is indeterminate or suspicious on the initial screening mammogram, our radiologist may recommend further diagnostic studies including additional views, ultrasonography or MRI in order to determine the cause of the area of concern on the screening exam. Diagnostic mammography is also used to evaluate a patient with abnormal clinical findings-such as nipple discharge, breast lump or nipple retraction that have been found by the woman or her primary doctor.
Baylor Radiologists uses several advanced technologies including full-field digital mammography and computer-aided detection (CAD). Our radiologists are board-certified physicians with subspecialty expertise. We are committed to serve our patients with the highest standard of care.
Clinical Instructions
- Do not wear deodorant, talcum powder or lotion under your arms or on your breasts on the day of the exam. These can appear on the mammogram as calcium spots.
- Describe any breast symptoms or problems to the technologist performing the exam.
- If possible, obtain prior mammograms and make them available to the radiologist at the time of the current exam.
Ultrasound
Ultrasound is primarily used is to help identify and diagnose breast abnormalities detected by a physician or patient on a physical exam. It is also used to characterize potential abnormalities seen on mammography often times to determine if a potential breast abnormality is a benign cyst (fluid-filled) or is solid (which may be a non-cancerous lesion or a cancerous tumor). If a potential breast abnormality is visualized with ultrasound, a needle aspiration/core biopsy may be performed under ultrasound guidance. Ultrasound is often the initial imaging test for women younger than 30 years of age without or with pregnancy because ultrasound does not utilize ionizing radiation.
Breast MRI
MRI is a supplemental tool for detecting and staging breast cancer and other breast abnormalities. MRI may be used to evaluate abnormalities detected by mammography and/or breast ultrasound. In certain situations such as in high risk patients or women with dense breast tissue, breast MRI can also be used as a screening tool. Current indications for breast MRI include:
- Determine tumor extent for example to see whether cancer detected by mammography or ultrasound has spread further in the breast or into the chest wall.
- Search for multiple tumors prior to breast conservation surgery.
- Determine breast implant integrity
- Determine how much cancer has spread beyond the surgical site after a breast biopsy or lumpectomy.
- Distinguish between scar tissue and recurrent tumors.
- Screening women at high risks for breast cancer.
Clinical Instructions
A pregnancy test may be necessary prior to your MRI exam. The risks to a fetus are unknown. Therefore, pregnant women should not have an MRI exam unless the potential benefit from the MRI is determined to outweigh the potential risks. If you have minor claustrophobia (fear of enclosed spaces) or anxiety, you may want to request a prescription for a mild sedative from your physician. If you have an allergy of any kind such as hay fever, hives, allergic asthma, or allergy to food or drugs, please indicate that on your history form as rarely, some individuals can have an allergy to gadolinium. However, gadolinium does not contain iodine and is less likely to cause an allergic reaction as compared to the CT contrast that contains iodine. The technologist and radiologist should also know if you have any significant health problems. Some conditions, such as kidney disease and sickle cell anemia, may prevent you from having an MRI with contrast material.
Metal and electronic objects can interfere with the MRI’s magnetic field and are not allowed in the exam room. These items include:
- Jewelry, credit cards, watches, hearing aids, all of which can be damaged.
- Pins, hairpins, metal zippers and similar metallic items, which can distort MRI images.
- Removable dental work.
- Pens, pocketknives and eyeglasses.
In most cases, an MRI exam is safe for patients with metal implants, except for a few types.
Tell the technologist if you have medical or electronic devices in your body, such as artificial heart valves, implanted drug infusion ports, implanted electronic devices, artificial limbs or metallic joint prostheses, implanted nerve stimulators, metal pins, screws, plates or surgical staples.
Metal objects used in orthopedic surgery usually pose no risk during MRI. However, a recently placed artificial joint may require the use of another imaging procedure such as CT. If there is any question, an x-ray may be taken to detect the presence of any metal objects.
Breast Biopsy
Percutaneous breast biopsy under imaging guidance (x-ray, ultrasound or MRI) is an alternative to open surgical biopsy for the evaluation of indeterminate or suspicious breast lesions. Stereotactic biopsy uses digital mammography along with computer target localization most commonly to biopsy suspicious or indeterminate calcifications in the breast. Occasionally, it can also be used to biopsy masses or lesions not seen under ultrasound.
Ultrasound is also commonly used to guide biopsy of breast lesions visible on ultrasound. It may be performed with either a large hollow needle (automated core breast biopsy) or a vacuum assisted device which grabs the tissue with a vacuum and then uses a cutting tool to free the tissue from the breast. Breast lesions seen best on MRI can be biopsied under MRI guidance.
When it is necessary to do an open surgical biopsy or surgically remove a previously biopsied mass or group of calcifications, a guide wire first is passed directly into the mass or cluster of calcifications to help the surgeon locate the lesion. This procedure may be guided by mammography, ultrasound or MRI.
Clinical Instructions
If you are taking aspirin or a blood thinner, your physician may want you to stop seven days in advance of the biopsy.